Lung Cancer Treatment
Treatment for lung cancer, a type of cancer that forms in the lungs and is the leading cause of cancer-related deaths worldwide, can vary depending on factors such as the cancer stage and cell type, patient age, and overall prognosis. After a lung cancer diagnosis, the best forms of treatment are discussed between you and your care team.

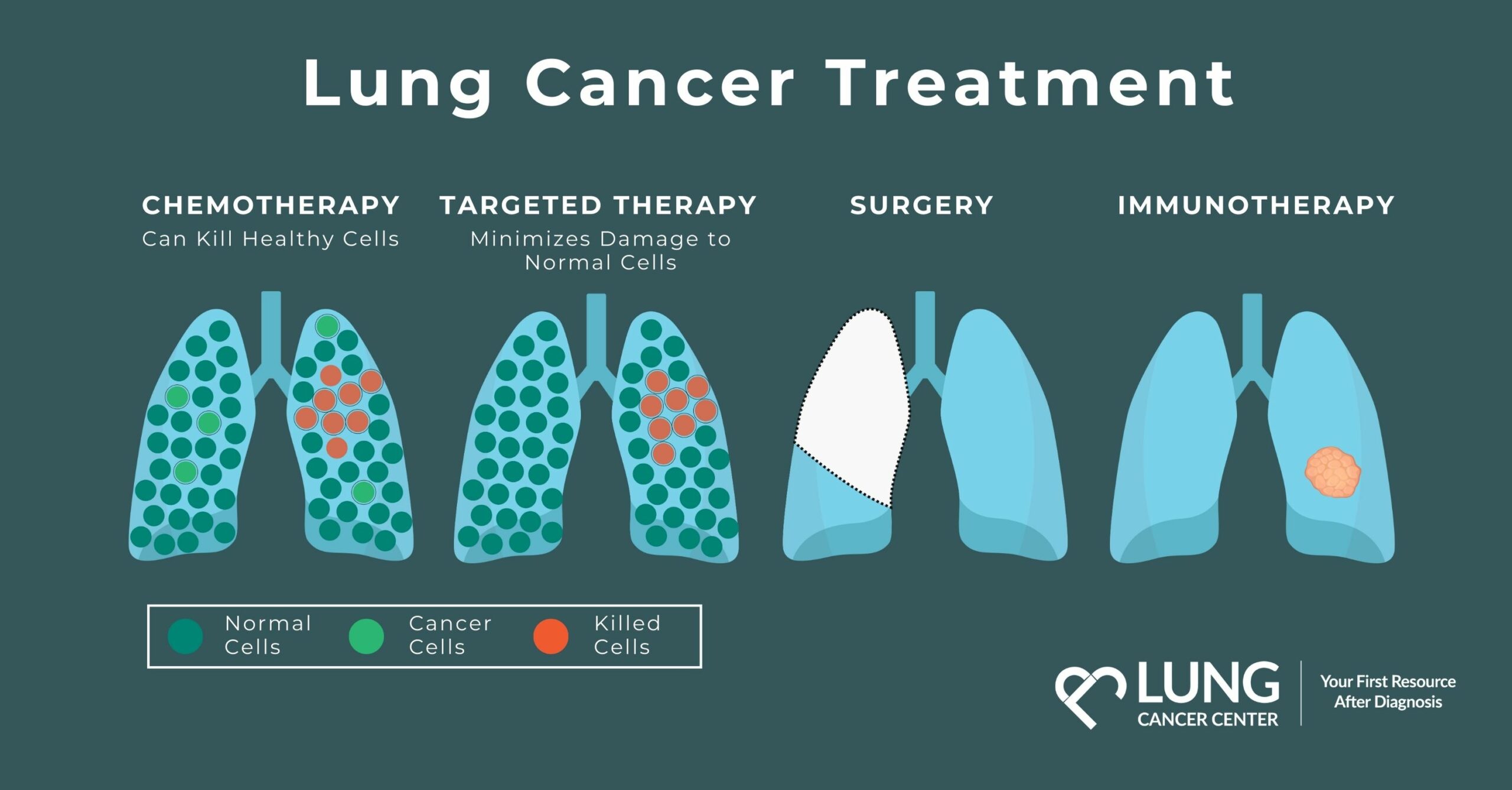
Treatment Information for Lung Cancer
Lung cancer treatment options are a significant concern among patients living with the complex disease. Treatments are constantly evolving as breakthroughs in science and technology pave the way for new approaches. You may feel like you have to navigate a tough path to treatment with the overwhelming variety of available options. Each method comes with its own set of potential benefits and side effects, making it challenging for you and your family to weigh the pros and cons effectively.
Emerging lung cancer treatments offer personalized approaches and improved outcomes. The introduction of new therapies to fight lung cancer has helped improve survival rates for lung cancer, with a five-year survival rate increase from 17.2% in the early 2000s to 21.7% in recent years, according to the American Cancer Society.
Whether you choose to undergo standard treatments for lung cancer or participate in a novel clinical trial, your team of healthcare professionals will offer their guidance and expertise to help you make treatment decisions along the way.
Lung Cancer Treatment Types
Globally, lung cancer affects millions of people each year. Every diagnosis is broken down into lung cancer types, including non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC). It is important to determine the type of lung cancer because that can affect treatment options and outcomes. Specific characteristics of each lung cancer type, as well as individual factors, can influence how your oncologist targets your treatment plan to address your specific needs. Certain therapies, even though they may be better at curing than other choices, could be too strong for older or less healthy patients. Onocoligists consider these factors when forming a customized treatment plan.
Lung cancer treatment plans often include various types of treatments, including surgery, chemotherapy, radiation therapy, immunotherapy, or targeted treatments. The selection and combination of these treatments differ for everyone.

Surgery for Lung Cancer
Surgery for lung cancer involves the removal of the tumor or affected part of the lung and can vary in recovery time, which may span from weeks to months. Potential side effects may include pain, fatigue, and shortness of breath. Scarring can impact lung function but is usually manageable. Surgery is more common in early stages as a curative approach. In advanced cases, it may serve as part of a broader treatment plan.
Different types of surgery, including minimally invasive approaches or open surgery, require varying recovery times and care. Decortication, is one of the more invasive methods which is a surgical procedure that removes the fibrous tissues in the pleural lining. Cases of right upper lobe cancer may require surgical procedures such as lobectomy or segmentectomy as primary approaches to eliminate the affected portion or entirety of the lung.
While lobectomy ensures the complete removal of the entire affected lobe, segmentectomy is a more conservative option, preserving more lung tissues. Lung cancer surgeons evaluate these factors to determine the most suitable surgical procedure. Some procedures for SCLC and NSCLC are:
- Lobectomy
- Pneumonectomy
- Segmentectomy
- Sleeve resection

Chemotherapy for Lung Cancer
Chemotherapy is a standard lung cancer treatment involving the use of drugs to target and kill cancer cells throughout the body. The recovery time after chemotherapy sessions usually involves a cycle of treatment followed by a period of rest to allow the body to recover from the side effects. Common side effects of chemotherapy include fatigue, nausea, hair loss, and a weakened immune system.
The intensity and duration of these side effects depend on the stage of lung cancer. In early stages, chemotherapy may be used in combination with surgery or radiation to eliminate any remaining cancer cells. In advanced stages, where the cancer has spread to other areas, chemotherapy may be a primary treatment to shrink tumors and control the disease. Treatment plans involving chemotherapy are individualized to each patient, considering factors like overall health, treatment goals, and specific lung cancer types. Chemotherapy is administered in one of two ways: systemic and intraoperative. This is an important distinction in immunotherapy vs chemotherapy.
Systemic chemotherapy means that medication is used throughout the whole body. In this process, the chemo medication used can’t distinguish between healthy and cancerous cells and attacks the entire body. In intraoperative chemotherapy, chemo is applied directly to areas where surgeons have operated and removed tumors. Ultimately, this relieves some of the discomforts that systemic chemotherapy can cause. Common chemotherapy medications include:
- Cisplatin
- Carboplatin
- Pemetrexed
- Vinorelbine

Radiation Treatment Options
Radiation therapy is a common lung cancer treatment option, utilizing high doses of focused radiation to target cancer cells. The recovery time after radiation treatment ranges from a few weeks to months. Common side effects vary by stage but can include skin changes, chest discomfort, and fatigue.
Radiation therapy types can be used in combination with surgery in early stages or as palliative care in advanced stages. When treating SCLC or NSCLC, oncologists can use radiation to shrink tumors and kill cancerous cells. External beam radiation therapy (EBRT), the most common form of radiation, involves a concentrated beam to target the tumors without affecting the surrounding area. EBRT is divided into small sessions lasting only a few minutes, several times a week for several weeks (as determined by a specialist). However, newer techniques can be used and affect the number of sessions a patient goes through. These techniques include:
- Intensity-modulated radiation therapy (IMRT)
- Stereotactic body radiation therapy (SBRT)
- Three-dimensional conformal radiation therapy (3D-CRT)

Immunotherapy Survival Rates
Immunotherapies for lung cancer involve the use of medicine to boost your immune system. While immunotherapy for lung cancer is not curative, this treatment modality has improved survival and reduced symptoms in many patients. Recovery time after immunotherapy is minimal compared to standard treatments like chemotherapy or surgery but can cause mild side effects. Some patients experience fatigue, skin reactions, or immune-related issues.
The negative side of traditional chemotherapy is that it cannot target cancer cells specifically. In most cases, it is administered systemically and so attacks the entire body, potentially weakening the individual who is simply trying to treat their cancer. This is where immunotherapy can help and. Immunotherapy boosts the body’s natural immune system to help fight cancer. Also, this helps patients who may not be as receptive to more aggressive treatments (such as surgery) and helps them fight their cancer in a way that is less harmful to the body.
While still considered an “emerging lung cancer treatment,” immunotherapy and its related medications has shown positive effects in the long term, with less hazardous side effects.
For more information, fill out a free case evaluation form today.

Targeted Therapy – Medications and Treatment
Recent developments in lung cancer treatments have focused on targeted therapy, a method involving medications that specifically target genetic or molecular abnormalities causing cancer growth. Targeted therapy medications, including Bevacizumab and Ramucirumab, are designed to spare healthy cells while interrupting the growth and function of these specific abnormalities.
Targeted therapy treatment for lung cancer is most commonly used to treat non-small cell lung cancer with specific genetic mutations, such as EGFR, ALK, and MET exon 14 skipping. Mild to severe side effects of targeted therapy can occur, including dry skin, high blood pressure, skin rash, or swelling. Targeted therapy uses angiogenesis inhibitors to block the growth of cancer cells. These inhibitors are administered in cases of advanced lung cancer for NSCLC. These inhibitors include Bevacizumab and Ramucirumab.
Aside from angiogenesis inhibitors, there are other medications in targeted therapy that target mutations in the epidermal growth factor receptor (EGFR). EGFR is responsible for cell activity, including growing and dividing. In people with NSCLC, the cancerous cells can have too much EGFR, which will, in turn, cause them to grow much faster than healthy cells in the body. Medications that inhibit cells with too much EGFR do so by looking for mutations in that gene. These medications include:
- Afatinib
- Dacomitinib
- Erlotinib
- Gefitinib
- Osimertinib

Radiofrequency Ablation for Lung Cancer
Radiofrequency ablation (FRA) is a newer and minimally invasive treatment option for lung cancer that employs high-frequency electrical currents to heat and destroy cancerous cells. Recovery time after RFA is relatively shorter compared to traditional surgery, ranging from a few days to weeks. Common side effects are generally mild and may include chest and lung pain or discomfort or a temporary cough. In cases where surgery is not suitable, RFA may be utilized as a primary treatment for small tumors. In late stages, RFA can provide relief from symptoms and improve the patient’s quality of life.
Radiofrequency ablation (RFA) can be used either in a curative or palliative way. RFA is especially useful for individuals who may need to avoid aggressive surgery. For the procedure, surgeons, guided by a CT scan, will insert a needle-like probe through the skin and into the tip of the tumor. Then, an electric current is used to heat the probe and the tumor, destroying the cancerous cells.

Palliative Care – Relieving Cancer Pain
While standard cancer treatments address the disease itself, palliative care addresses other issues, including nausea, fatigue, and shortness of breath, aiming to improve quality of life. Palliative care helps patients, especially those in later stages, manage symptoms and discomfort. Palliative care techniques depend on the patient’s needs but can include pain management and symptom control strategies. This type of treatment typically involves the use of medications or physical therapy in combination with other treatments.
While the above forms of lung cancer treatment are primarily used as curative therapies, there are times when oncologists and surgeons use them as palliative care. Palliative care is any treatment that is used to relieve symptoms of lung cancer or side effects of its treatment. This can mean using radiation to shrink tumors that may be causing discomfort or even surgery to alleviate the pain of complications like pleural effusion.
Best Lung Cancer Hospitals for Treatment
Several globally recognized hospitals and medical centers offer exceptional lung cancer treatment and care. The MD Anderson Cancer Center in Houston, Texas, for example, is well-known for its wide range of treatment options and distinguished healthcare providers in its dedicated lung cancer program.
Other medical centers for lung cancer, including Memorial Sloan Kettering Cancer Center in New York City and Gustave Roussy Cancer Campus in France, offer comprehensive lung cancer care from some of the best experts and specialists in the field.

Where to Find Lung Cancer Clinical Trials
Each year, clinical trials for lung cancer are conducted to improve existing treatments or discover new approaches. Patients may choose to participate in a clinical trial to hope for improved outcomes or reduced side effects. For individuals who may not respond well to conventional treatments, clinical trials provide an opportunity to explore alternative and potentially more effective treatments. You can find ongoing clinical trials for lung cancer with criteria specific to your requirements using various platforms, such as ClinicalTrials.gov, or medical center websites like MD Anderson Cancer Center and Sloan Kettering Cancer Center. You can also consult with your healthcare provider, oncologist, or clinical trial coordinator for personalized recommendations.
Clinical trials are special rounds of medication and combination therapies that have yet to be approved by the FDA and, sometimes, not yet tested on humans. While these lung cancer treatments can have promising results, not everyone may qualify. Before looking for a clinical trial, a person with lung cancer must consult their oncologist to see if clinical trials suit their prognosis. If an oncologist approves it, the individual will go through an interview process to learn if they are the right fit for the trial. Factors that can determine if someone is a right fit for a trial can include:
- Age
- Sex
- Family history
- Personal medical history
- Current medications
- Current Smoker or Not
Alternative Cancer Treatments
Alternative lung cancer treatments, or non-conventional therapies, involve a variety of techniques used alongside standard approaches. Some alternative approaches include mind-body techniques like meditation and yoga to reduce stress, and physical techniques like acupuncture to reduce nausea and pain. Patients should always communicate openly with their healthcare team to address potential interactions or mental health conflicts between alternative and conventional treatments. Complementary therapies are mental to work in combination with standard treatments.
Lung Cancer Life Expectancy with Treatment
Lung cancer life expectancy with treatment varies by stage and type. Early-stage lung cancer cases are often eligible for potentially curable surgical procedures when combined with chemotherapy or radiation. The overall health of the patient, age, and the extent of the disease influence the outcome. Other factors such as the presence of genetic mutations can infusion life expectancy.
Lung Cancer Treatment Research
Researchers are always working to improve treatments for lung cancer while focusing on improving outcomes and quality of life for patients. Major focuses of lung cancer research involve early detection methods using molecular biomarkers found in blood and the combination of immunotherapy drugs with chemotherapy to shrink tumors.
Research on new surgical approaches, including robotic-assisted surgery and video-assisted thoracic surgery, continues to enhance the precision of minimally invasive treatment options. Robotic-assisted surgery utilizes sophisticated robotic systems controlled by surgeons. This technology can make surgeries less painful, cause less scarring, and help patients recover faster.
Post Cancer Treatment Care
As a lung cancer survivor, overcoming challenges and celebrating small wins are not new concepts, and they are just as important in the recovery process. Post-cancer treatment care for lung cancer patients is a crucial phase of recovery that can include regular follow-up appointments and lifestyle adjustments to support well-being and resilience. It is essential for people who survive lung cancer to check up with their doctor regularly. Lung cancer survivors could be at a higher risk of developing a new disease or a second cancer.
Survivors of SCLC and NSCLC are most at risk of developing the other form. Other cancers they are likely to develop include:
- Esophageal cancer
- Larynx cancer
- Mouth or throat cancer
- Thyroid cancer
It is also possible, though less likely, that they could develop cancer in a different part of the body (such as the stomach, colon, and pancreas). Regular screenings and early detection are critical for any cancer survivor. If you have gone into remission, talk with your doctor about your chances of developing a second cancer.
Living Life After Treatment
After lung cancer treatment, patients typically attend regular appointments to monitor side effects and go over results from screenings done regularly to detect potential recurrences. During these appointments, the healthcare team may conduct physical examinations, imaging tests (such as CT scans or X-rays), and blood tests to monitor for any signs of health issues.
Life after treatment may involve prioritizing physical activity and a balanced, enriching diet. Aim for a diet consisting of fruits and vegetables, lean protein, whole grains, healthy fats, dairy, and lots of hydration. Engaging in gentle and easy exercises can be beneficial for cancer survivors. Easy exercises that can be adapted based on individual comfort and energy levels include:
- Walking
- Stretching
- Yoga
- Swimming
- Chair Exercises
- Cycling
- Breathing Exercises
Mental health support is essential and can be attained by connecting with support groups or seeking counseling. This type of support can aid in processing emotions and navigating uncertainties. Preserving your resilience by prioritizing your health and your well-being can lead to a fulfilling and meaningful life, no matter where you are in your survivor journey.
Affording Expensive Lung Cancer Costs
Even with health insurance, the cost of lung cancer care can still add up. Affording the sometimes substantial costs associated with lung cancer treatment places a burden on patients and their families. To manage and reduce these costs, you can explore several strategies. Although lung cancer can be physically and emotionally devastating, it does not necessarily have to lead to financial distress. Reviewing insurance policies to understand coverage for various treatments and potential out-of-pocket expenses can help you prepare for and manage expenses. Open communication with healthcare providers or social workers about financial concerns can lead to referrals to assistance programs that may be available to help.
Receiving Financial Assistance for Lung Cancer Treatment
Navigating the financial challenges of lung cancer treatment can be overwhelming, but several resources exist to provide assistance and ease the burden of medical costs, including medications, surgeries, and other aspects of care. Various foundations, agencies, and patient advocacy groups offer financial support to lung cancer patients, guidance on accessing assistance, and help navigating the complexities of insurance coverage. Some helpful resources include:
American Lung Association: Provides information and resources, including possible financial assistance, through their Lung HelpLine and online support communities.
LUNGevity Foundation: Offers financial assistance through the Lung Cancer HELPLine and the Lung Cancer Financial Assistance Program for treatment-related expenses.
Legal assistance may be accessible if you or a family member developed lung cancer from exposure to asbestos, a naturally occurring material used in a wide range of products. Lung cancer lawsuits are filed by lawyers and attorneys against the manufacturers of products containing asbestos. Most cases reach a settlement agreement, ranging from thousands to millions of dollars depending on factors like specific asbestos-containing products involved, duration and intensity of exposure, and the impact on the individual’s health.
Lung cancer patients across the country may be eligible for financial assistance for both non-small cell lung cancer or small cell lung cancer if their diagnosis is linked to asbestos exposure. Our team can guide you in the compensation process. Contact us to get assistance.


