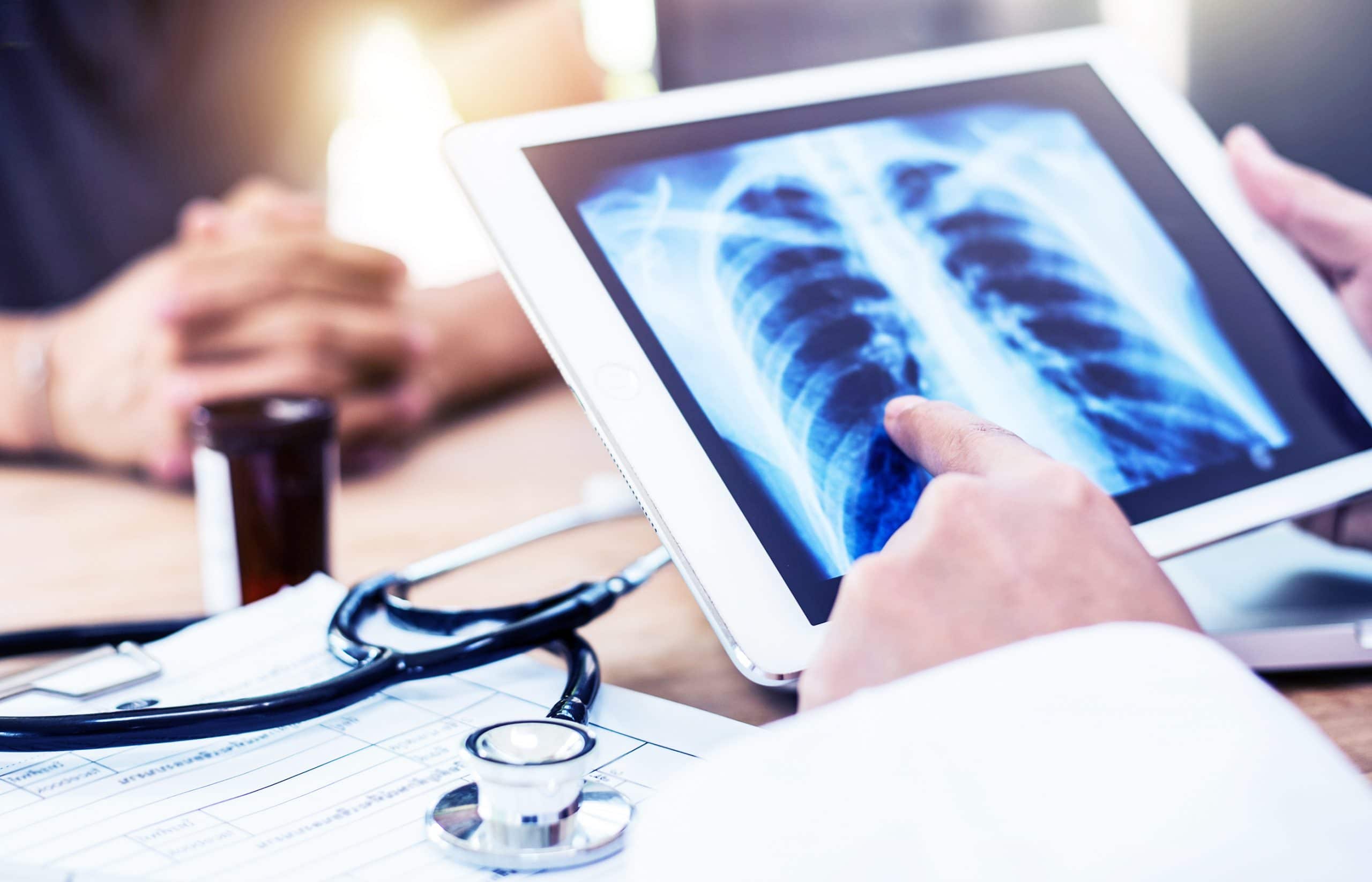
Lung Cancer Diagnosis
A diagnosis is important in the official identification of lung cancer. Once a diagnosis has been made, a doctor can then develop a treatment plan. Your doctor must give you a diagnosis before assessing the prognosis.
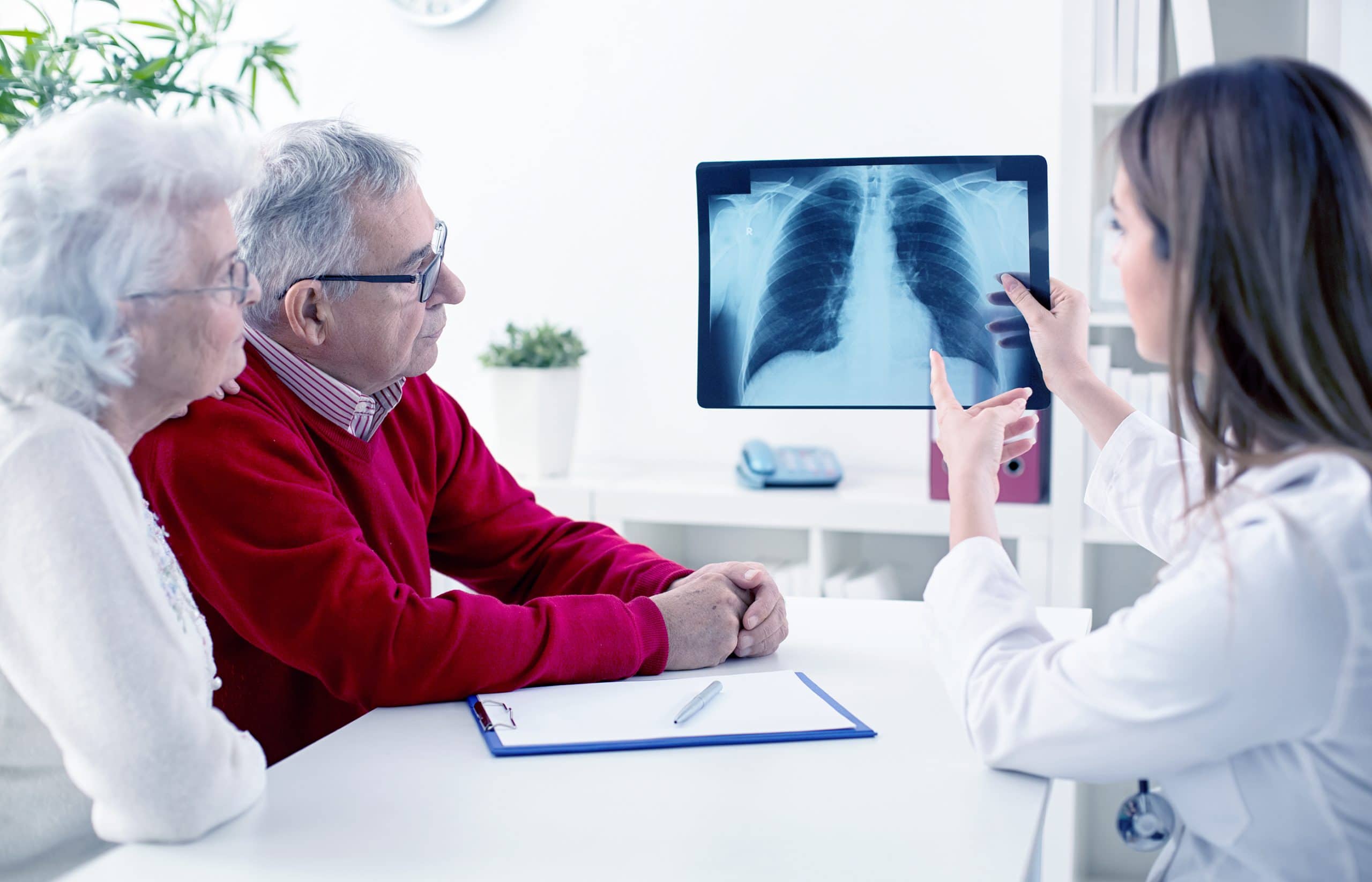
What Is a Lung Cancer Diagnosis?
Getting a diagnosis from a doctor is like unlocking the mystery behind your symptoms. Sometimes, exposure to harmful stuff like toxins can lead to serious conditions like lung cancer. If you’ve spent years around hazardous substances, your risk of developing this and other illnesses might go up, underscoring the importance of early detection.
In this blog, we’re diving into the critical importance of a lung cancer diagnosis. Early screening is a game-changer for most people, often resulting in a more optimistic diagnosis. When you catch it sooner, you open doors to a wider range of treatments—options that can really make a difference, whether it’s about curing the disease or easing its impact. Learn how managing lung cancer becomes way more manageable when you receive a lung cancer diagnosis.
Lung Cancer Diagnosis Versus Screening
Doctors rely on screening and diagnostic tests for a dual purpose. Screening tests are the frontline detectives, scanning through a large pool of individuals to spot potential early signs of a disease or identify risk factors. Once something triggers concern, a diagnostic test for lung cancer steps in to definitively confirm the presence of the disease and craft a tailored treatment approach.
How to Detect Lung Cancer
Signs of tumors in the lungs may include shortness of breath or wheezing, coughing up blood, and a recurring cough. If you are experiencing these lung cancer symptoms, you may want to consult with your doctor about a lung cancer detection test.
Detecting lung cancer involves several diagnostic methods. Imaging tests such as lung cancer X-rays, CT scans, and MRIs provide detailed visuals of the lungs, enabling the identification of any anomalies. Should an abnormality arise, a biopsy becomes necessary—a procedure in which your doctor extracts and examines a small tissue sample under a microscope to confirm the presence of cancer cells. Sputum cytology, analyzing lung cancer phlegm mucus from coughed-up material, assists in identifying cancerous cells. Blood tests, while not conclusive, may show lung cancer biomarkers that provide supplementary insights. Additionally, screening programs, notably low-dose CT scans, are recommended for individuals at higher risk, facilitating the early detection of potential lung cancer. Seeking medical attention upon noticing symptoms or having risk factors is crucial for timely intervention and improved outcomes.
Get the Help You Need
Getting a Lung Cancer Diagnosis
Those with concerns about lung cancer should visit their primary physician for a screening. If the doctor decides a diagnostic test is necessary, they will administer the appropriate tests on the patient. There are several diagnostic tests for lung cancer that medical professionals can give depending on the patient’s symptoms. After the diagnosis is made, the doctor can begin developing a treatment plan in expectation of how the cancer will develop (also known as its prognosis). Diagnostic tests used for cancer patients include:
Computed Tomography (CT) Scan
CT scans, also known as computed tomography scans, are a non-invasive diagnostic procedure that utilizes a series of X-ray images taken from multiple angles around the suspected area to create a detailed and three-dimensional image of the inside of the body. This advanced imaging technique allows doctors to get an up-close look at bones, blood vessels, and soft tissues inside the body. CT scans are particularly useful in detecting lung cancer, as they provide a more complete and detailed look than X-rays alone, enabling doctors to diagnose and treat the disease more effectively. The images produced by lung cancer CT scans are processed using computer software, which arranges them to create a highly detailed and accurate picture of the area being examined.
Positron Emission Tomography (PET) Scan
Another imaging test, a PET scan, helps show how tissues and organs are functioning. First, the doctor administers a radioactive drug known as a tracer to highlight the target area and get a better look. The tracer can be injected, swallowed, or inhaled depending on the area it must go. It builds up in areas of the body that have excessive levels of chemical activity, which correlates with the activity in diseased areas.
Bone Scan
Your doctor can detect changes or abnormalities in bones with bone scans. A bone scan is also known as a radionuclide scan, bone scintigraphy, or nuclear medicine bone scan. Irregularities detected in the scan can be called hot spots but don’t always mean cancer. A CT scan may be needed to detect illness further if a bone scan comes back with unclear hot spots.
Lung Cancer MRI
MRI scans are a type of medical imaging that uses radio waves and strong magnets to create highly detailed images of soft tissue. Similar to CT scans, they are capable of producing detailed images of the tissue in the chest cavity. Their primary use is to determine whether lung cancer has spread beyond its initial site. With the help of MRI scans, doctors can get a better understanding of the extent of the cancer and develop a more effective treatment plan.
Bronchoscopy and Biopsy
Bronchoscopy and biopsy are important diagnostic procedures used to identify lung cancer. During a bronchoscopy, doctors insert a thin, flexible tube equipped with a camera through the mouth or nose and guide it into the lungs. This allows doctors to visually examine the airways and obtain tissue samples (biopsy) from suspicious areas within the lungs. The collected tissue is then analyzed under a microscope to determine if cancerous cells are present. These tests are crucial in confirming the presence of lung cancer, identifying its type, and guiding subsequent treatment decisions. They provide a direct and precise way of obtaining tissue samples for accurate diagnosis and planning appropriate treatment strategies.
Lung Cancer Misdiagnosis
Medical professionals can sometimes mistake lung cancer for a rare form of cancer known as pleural mesothelioma. Mesothelioma is similar to lung cancer in that it develops in the lungs but is different in that tumors will metastasize (grow) in the lining of the lungs or the pericardium instead of within the lungs themselves. If a doctor misdiagnoses your illness, there’s no way for you to know until you get a second opinion.
Have a detailed discussion with your doctor on your screening and diagnosis results. If your doctor determines you have lung cancer and you have any concerns with the validity of the diagnosis, you can always (and have the right to) get a second opinion from another doctor. Your doctor can also inform you of the steps to take that may help improve your prognosis.
For more information, fill out a free case evaluation form today.
Some Questions to Ask Your Doctor
For most people, visiting the doctor to talk about potential illnesses can be intimidating. In stressful situations, it can be helpful to have a list of prepared questions that are important to ask your doctor before and after your diagnosis so you don’t forget anything.

Before your diagnosis:
- How common is lung cancer?
- What types of lung cancer are there?
- What are the causes? What caused my disease?
- What are my risk factors? How high of a risk am I for getting lung cancer? Why?
- What type of screening and diagnostic tests do you recommend for my situation? Why?
- How long does it take to get my results back?
- What can I expect from this test?

After your diagnosis:
- What does my diagnosis mean? What type of lung cancer do I have?
- What treatment plan do you recommend, and how will this affect my day-to-day?
- How much does lung cancer treatment cost? What does my insurance cover?
- What are the symptoms I may experience?
- What other resources are available to me?
- What are clinical trials, and can these help my situation?
- What clinical trials are in my area?
- What lifestyle habits will aid me through treatment and after?
- Is there any integrative medicine that can help ease the side effects of treatment?
- Do I need a second opinion?
Next Steps
If you suspect that you may have symptoms of lung cancer, it is essential to seek medical attention as soon as possible. It is important to convey all the details of your situation to your doctor and explain why you believe you may be at risk. This way, your doctor can accurately assess your risk level and determine the best course of action for your specific needs. Remember, each person’s case is unique, and it is crucial to address any potential health concerns proactively. Don’t hesitate to schedule an appointment with your doctor to discuss your concerns and receive the appropriate screening and diagnosis.