What Is Early Screening?
Early screening for lung cancer takes place before the patient has any symptoms. Results can help patients survive cancer or live longer with treatment.
Early Screening for Lung Cancer
Unlike testing, early screening for a disease occurs before the patient has any symptoms. When screening for cancer, early detection can encourage patients to seek treatment sooner when more curative options are available. The earlier cancerous cells are detected, the easier they are to treat with radiation, chemotherapy, or surgery. Catching lung cancer in an early stage, before it has spread throughout the body, can increase a patient’s odds of survival and improve their prognosis.
Today, lung cancer is the leading cause of cancer-related death in the U.S., making up nearly a quarter of all cancer deaths in the country. In 2018, nearly a quarter of a million new cases of the disease were diagnosed, and over half a million people today live with a lung cancer diagnosis – meaning the majority of diagnoses occurred in the last few years. Recently, the large number of new cases can be attributed to the late onset of symptoms and limited treatment options available at later stages of the disease. Learn more to stay informed about the latest lung cancer screening recommendations and guidelines.
5-Year Survival Rate for Lung Cancer
While the current 5-year survival rate for lung cancer is about 18 percent, other cancers with widely available screenings have markedly higher survival rates – breast cancer, colon, and prostate have 5-year survival rates of 91, 66, and 99 percent, respectively. Thus, the importance of effective early screening methods is paramount in preventing cancer-caused death. Other common cancer screening methods include mammograms for breast cancer, colonoscopies to detect colon cancer, HPV tests for cervical cancer, and LDCT tests for lung cancer.
To date, only three screening tests have received serious attention from the medical research community: low-dose spiral CT (LDCT) scans, chest x-rays, and sputum cytology (i.e., phlegm cell analysis). Of the three, cancer professionals only recommend LDCT scans for the identification of early lung cancer and prevention of early death. Studies have shown that low-dose spinal CT scans reduce mortality rates by 20 percent.
It’s essential to understand the significance of early detection of lung cancer and the accepted screening methods if you or someone you know is at risk for lung cancer. The more you know about this topic, the better equipped you are to manage your health proactively.
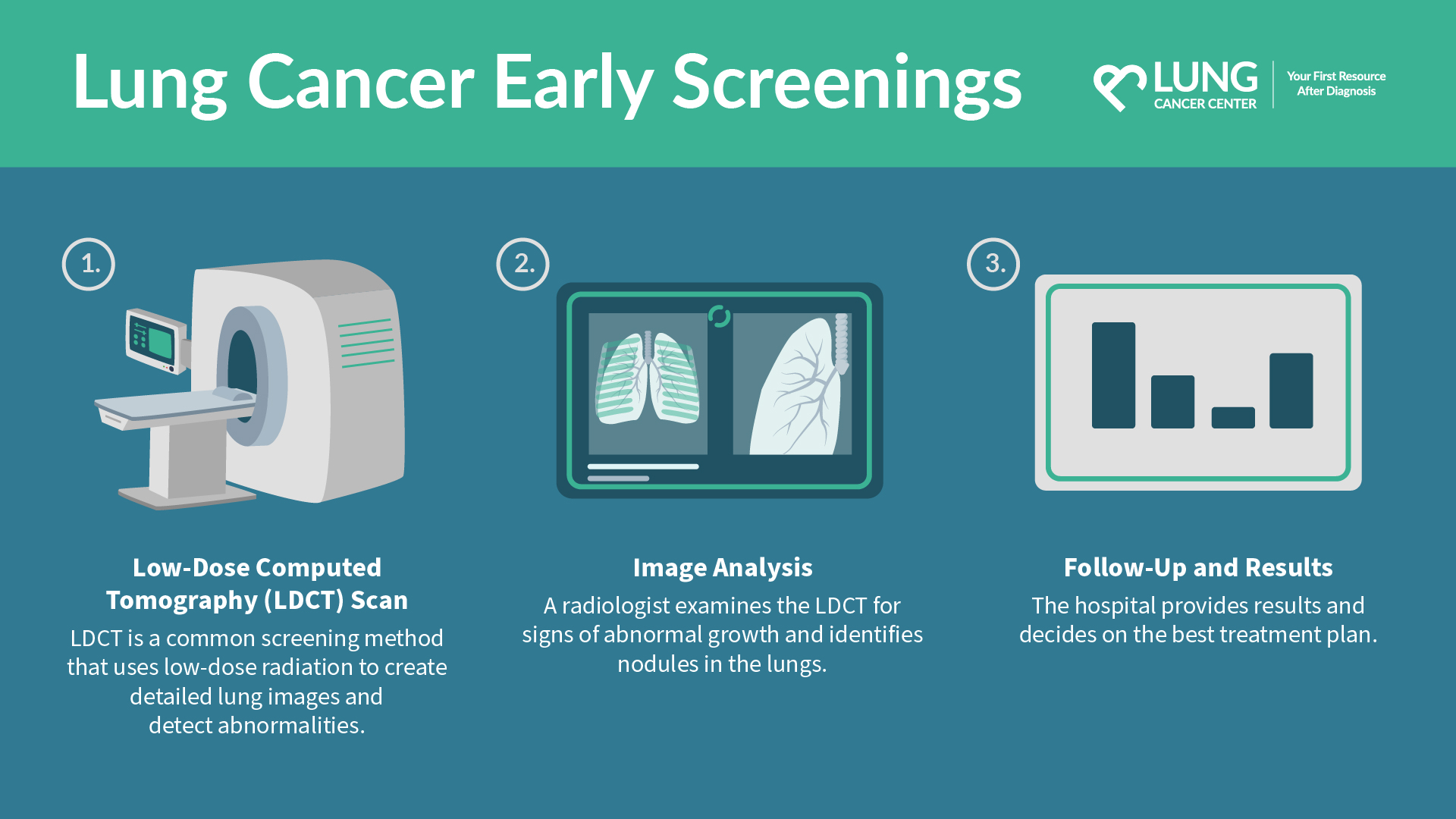
What Is an LDCT Scan?
A low-dose spiral computer tomography scan, or LDCT scan, is similar to a lung cancer x-ray, takes only minutes to administer, and is a painless procedure. Depending on the machine used, the patient either lays on a table and the scanner inserts their body into a large body scanner (like an MRI machine), or the scanner moves around the patient. The machine does not touch the patient but often makes soft whirring or clicking sounds.
The low-dose CT lung cancer screening is incredibly effective in detecting early signs of lung cancer, making it a vital tool in preventive healthcare. Its ability to capture detailed images with minimal radiation exposure significantly aids in identifying abnormalities at their initial lung cancer stages. Patients usually find the experience quite comfortable, as they are required to remain still while the machine operates around them, emitting only gentle sounds throughout the process.
How Accurate Is an LDCT?
LDCT scans give doctors detailed information about tumors from multiple angles. A single scan, through the use of a low dose of radiation, can reveal the size, shape, and location of any tissue or organ abnormalities in both two- and three-dimensions. Nonetheless, a single screening cannot differentiate between malignant and benign tumors. To properly diagnose mesothelioma, lung cancer, or other diseases, doctors typically need to conduct a series of tests and biopsies.
Studies have shown that low-dose CT scanning technology can detect up to 80% of lung cancers at an earlier stage, which can increase the chances of successful treatment. However, it’s important to note that a scan may not always detect lung cancer, which is why repeated screenings over time may be recommended, especially for those at higher risk of developing the disease. By undergoing regular screenings for lung cancer, individuals can take proactive steps toward their health and potentially catch any signs or symptoms of lung cancer early on.
Risks of Low-Dose Spiral Computed Tomography (LDCT)
While the early detection of cancer can lead to recovery from the disease, using LDCT scans for lung cancer screening can come with its own risks. For instance, repeated exposure to the radiation used in LDCT scans may cause lung cancer tumors to grow. Additionally, early screening for lung cancer does not help patients whose tumors have already spread to other places in the body (such as the lymph nodes or brain).
In other cases, false-positive as well as false-negative results can be among the risks for early lung cancer screening. In false-negative results, the screening fails to reveal the presence of cancer. Typically, this prolongs the amount of time it takes for patients to seek treatment, even when common symptoms of lung cancer are present. In false-positive results, the screening shows the presence of cancer when there is none. Often, this leads to additional testing and invasive surgical biopsies that generally require their own recovery time. In both situations, the patient is subjected to undue anxiety and stress – which can come with their own serious health complications.
Lastly, the risk of early screening for lung cancer is the overdiagnosis of illnesses that would have never become uncomfortable or life-threatening. For instance, an LDCT scan that shows a tumor in one lung may lead to a litany of aggressive and lengthy treatments like surgery, chemo, and radiation therapy. In most cases, it is impossible to know if withholding treatment helps patients live longer or not; researchers tend to believe that treatment may be more detrimental to patients with serious pre-existing medical problems related to smoking.
For more information, fill out a free case evaluation form today.
When Do You Start Screening for Lung Cancer?
For some patients, lung cancer screenings can lead to earlier diagnoses and a greater number of treatment options. However, according to the American Cancer Society, not everyone needs to undergo an LDCT scan for cancer screening. The ACS screening guidelines are based on aspects that put individuals at high risk or are a direct cause of lung cancer. For people between the ages of 55 and 74 years old and are in “fairly good health,” medical professionals advise patients to partake in yearly lung cancer screenings if:
- Is a current smoker or quit smoking in the past 15 years
- Have a 30-pack smoking history (i.e., the number of years the patient smoked multiplied by the number of packs per day)
- Are between 50 and 80 years old
- Enter smoking cessation counseling for current smokers
- Know the potential risks and benefits of LDCT scans
- Can visit an experienced lung cancer screening center
Because the average LDCT scan can cost 300 dollars or more (before insurance), many advise patients to make an appointment with their primary care physician for a referral to a specialist or prescription for screening based on a high-risk history.
When Should You Stop Screening for Lung Cancer?
The Centers for Disease Control and Prevention recommends that yearly lung cancer screening when the patient being screened:
- Is 80 years or older
- Has not smoked in 15 years or more
- Develops a health problem that makes them unwilling to have surgery
Choosing a Lung Cancer Screening Center
When considering a screening center for lung cancer detection, there are a few things to consider. Crucially, the medical centers you select should possess not only advanced equipment but also an adequately staffed and resource-rich infrastructure with innovative research. Emphasis on state-of-the-art multislice CT equipment capable of delivering high-quality, low-dose, non-contrast spiral CT scans is crucial. Collaboration with healthcare facilities housing specialized expertise in biopsy methods, board-certified pulmonologists, and thoracic surgeons dedicated to lung cancer further augments the screening center’s credibility. Following these criteria ensures a comprehensive approach to lung cancer screening and diagnosis.
Choosing a lung cancer screening center involves selecting a facility with advanced equipment and a well-staffed infrastructure. Look for centers with state-of-the-art multislice CT equipment and expertise in biopsy methods, supported by board-certified pulmonologists and thoracic surgeons. These criteria ensure a comprehensive approach to lung cancer screening and diagnosis. Early screening aims to prevent cancer death, so individuals with a history of smoking or toxin exposure should consult their doctor if they suspect symptoms. For assistance in connecting to a doctor or finding a screening facility, contact us for more information.

